
POSTPARTUM
We spent so much time planning for labour and delivery. But no one prepares you for your body or heart after you leave the hospital.
- @postpartumtogether
So let’s change that. Let’s consider both the moments before AND after your birth. Let’s set you up for success so that you feel held and confident during your postpartum journey as well.
Postpartum: The Fourth Trimester
While the big birth moment gets most of the recognition, it is SO crucial not to underestimate postpartum or forget to plan for it. Regardless of the path your birth takes, in the postpartum period you will be healing physically as well as undergoing incredible changes emotionally and hormonally. Don’t forget to dedicate time and planning to what your early days and weeks will look like, and where you will get your support from.
What To Expect When You’re Postpartum
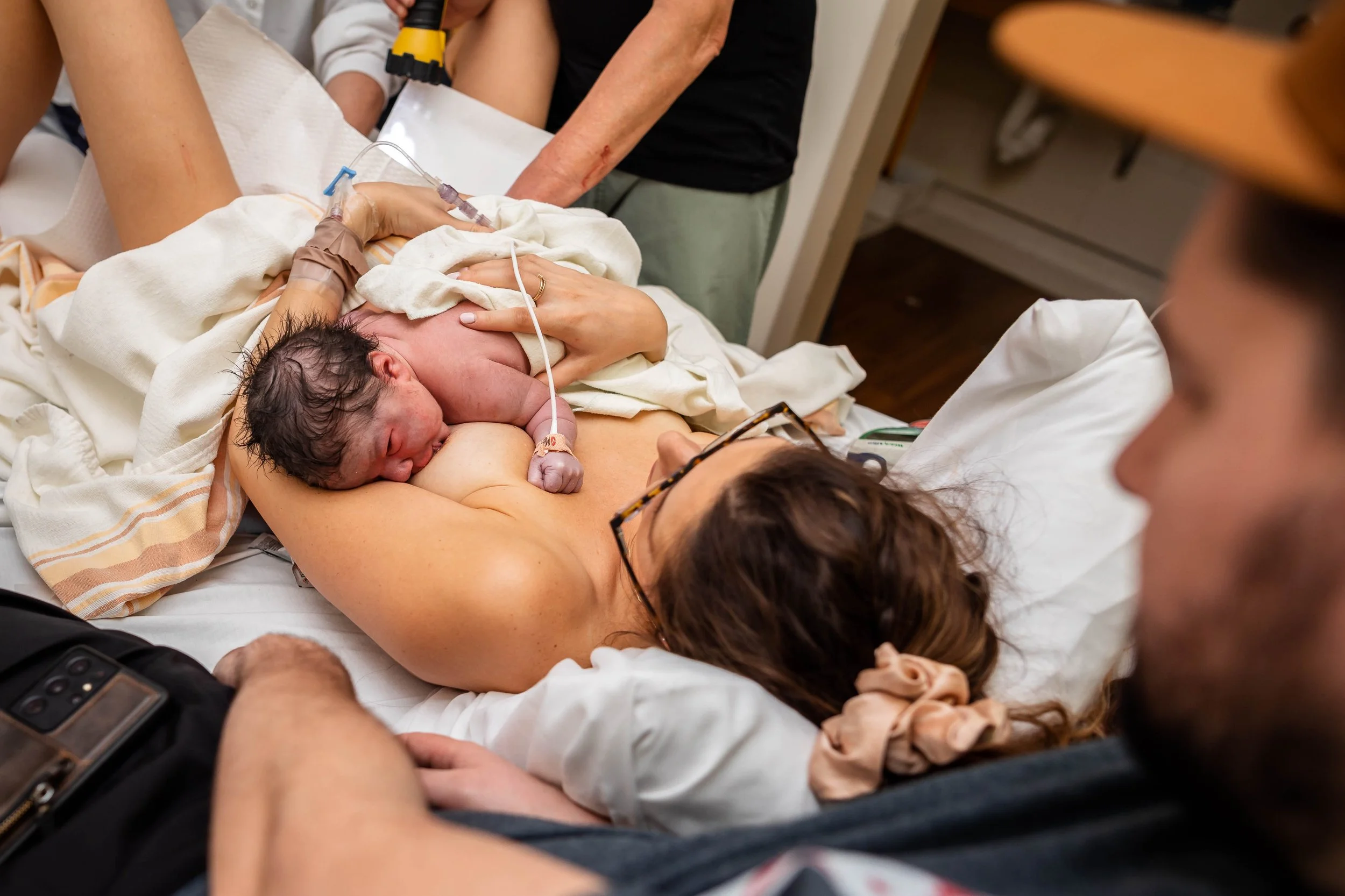
One of the most common things we hear from postpartum parents is that they wish someone had just prepared them more for what to expect postpartum. But it feels a little awkward, and a lot personal, and so it often gets skipped over. My aim here is to make this whole time period seem a little less unexpected, and a whole lot more supported. Here’s what I wish I knew.
First of all, this is a great overview of those first few weeks and some of the changes you may experience.
Some highlights?
Day 3 is often rough. Prepare for this. Do what you can to ensure good nutrition, enlist some help so you can grab a bit of extra sleep, and more than anything - be GENTLE with yourself. This is all new. Nobody expects perfection.
It will take some time before baby understands that there’s a day and a night and we prefer to sleep at night. For the first little bit, just go with it and sleep whenever you can. After the first few weeks, baby will adjust more to a routine.
Regardless of what kind of birth you had, you have a large wound where your placenta detached. While the size of it shrinks down with your uterus (those awful cramps are doing their job!), it is still raw, and you should treat it the same way you would any other wound - rest and care. It’s so tempting to push yourself if you are otherwise feeling pretty good, but go slowly or you risk starting back at square one.
Your emotions may be a roller coaster. That is normal. AND it is still important to monitor for moods and feelings that seem out of place. There is never any shame is seeking help to make sure you’re in the best hands possible.
-
This is most people’s primary concern, so let’s get it out of the way. If you had a vaginal birth there is a good chance that you will have tenderness in your perineum and vagina. If you had tearing or an episiotomy you will likely also have stitches. Your body has been through a lot - be gentle with it! Typically your stitches will dissolve and you may notice them on your pad or in the toilet. That’s ok and normal but can feel a little jolting.
You will be given a peri bottle postpartum - these are gold! Fill it with warm water and use it to rinse yourself after going to the bathroom. If you are experiencing a lot of stinging when you pee, you can also squirt warm water on yourself while you pee. The dilution can help a lot!
In the first day or so postpartum you may experience some swelling. This can be true even if you had a cesarean birth but pushed for a bit. You can use ice (a wetted and then frozen newborn diaper is perfect for this!) but my favourite for postpartum healing was witch hazel. Squirt some onto a pad, or you can make “padsicles” ahead of time using witch hazel and aloe vera. Like a little spa for your poor perineum!
-
Your lochia is the normal postpartum bleeding that you will experience after both a vaginal or cesarean birth. It will start out quite heavy, and then lessen over the next six weeks. You will be provided mesh underwear and pads in the hospital or birth centre, but many birthing people prefer to buy Depends underwear for a bit more of a feeling of security. Even better? A frozen pad inside the Depends that you can swap out when it starts feeling less effective. Leakproof AND soothing. You should alert your care provider if you are soaking a pad in less than an hour or passing clots larger than a grape after the first day. If your bleeding has started to taper off and then becomes heavier again, it means you are most likely exerting yourself too much, and it’s a sign to slow down.
-
Oh yes, we’re going there. Many people are concerned about their first bowel movement postpartum, and again - the lack of discussion about it doesn’t help.
One thing I like to remind clients is to treat your first BM the same way you do pushing - don’t do it until you’re really ready and your body is telling you it’s definitely time - and then follow your body’s lead. Stool softeners can help in the early days, but often this is more of a mind over matter problem than a physical one. Especially if you’ve had stitches, many people are afraid to push when the whole area still feels sensitive. To combat this, you can use a folded up piece of gauze or moistened toilet paper to provide gentle counterpressure on your perineum while you push. This can help you feel more supported and less worried about your stitches. Remember your labour breathing, and let your body do the work.
-
You’ve probably heard by now that there is a huge hormonal shift during your postpartum period. What you may not have considered is that this shift is also accompanied by a period of significant sweating. The combination of a drastic drop in estrogen alongside your body letting go of extra pregnancy fluids that it has held onto means you may find yourself frequenting waking up in a sweat. These typically taper off by around six weeks as your body stabilizes into its new normal.
-
With my first baby, I remember my mother in law asking me at about 3 days postpartum how my abdomen and ribs were feeling, and if I felt all “squishy” and I remember being simultaneously shocked that we were discussing such a personal thing, and also so SEEN. I don’t remember reading anywhere about this feeling prior to giving birth (and I was a doula!), and I was shocked by how empty and shifty everything felt after being all full of baby for nine months! We forget how much our organs and ribs move during pregnancy to make room, and also that everything doesn’t go back magically at once. For several weeks afterwards you may notice odd feelings of shortness of breath and even some nausea as all your insides go back to where they were meant to be! A belly band can do wonders for this. I got one after my third pregnancy and I wish I’d had it from the start!
Physical Postpartum Changes
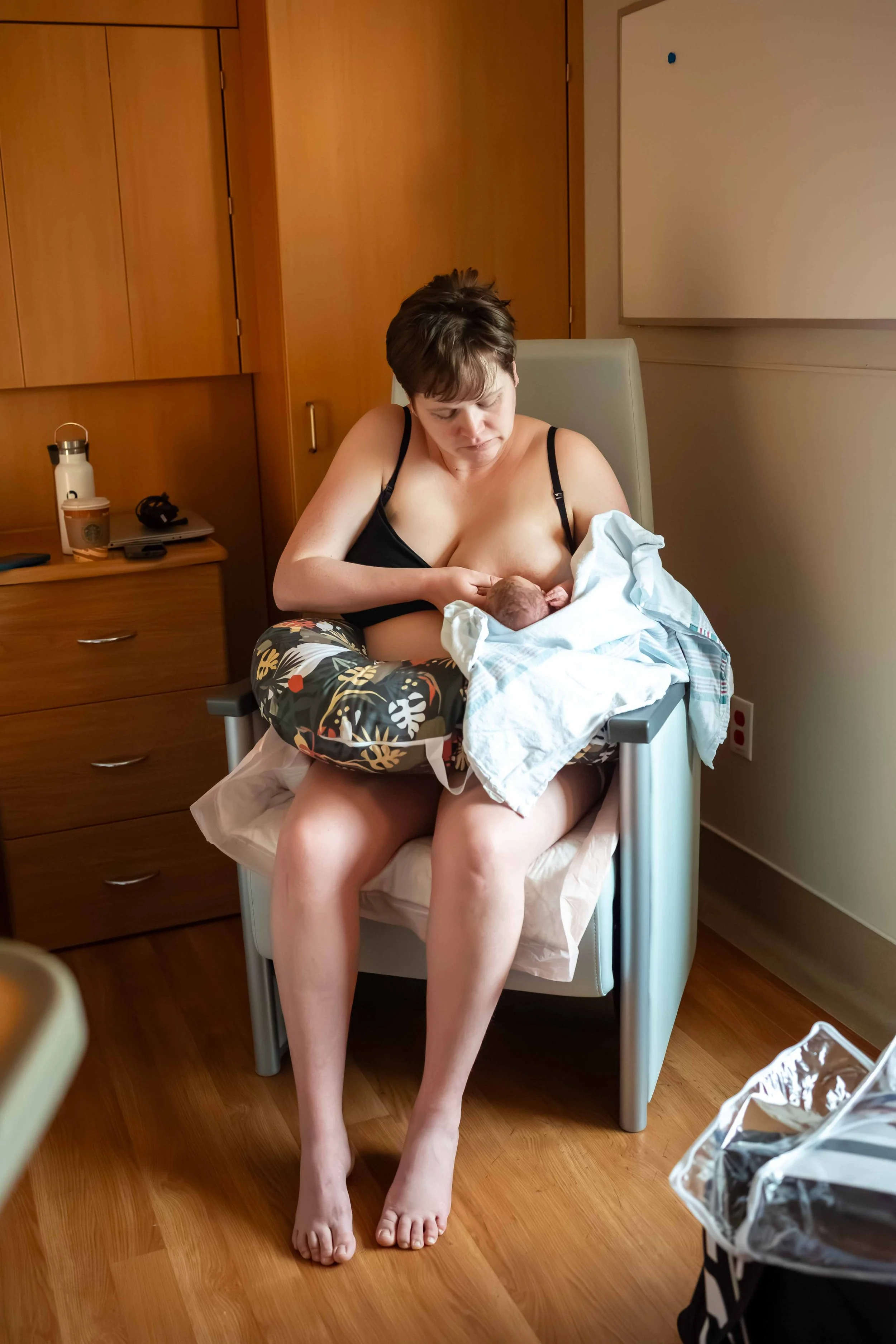
People want to hold the baby, not clean and cook, which is what I desperately need.
While the baby is of course the cutest part of postpartum, simply holding the baby doesn’t get done all the things you’re going to need. If you don’t think of these things ahead of time, you may find yourself exhausted, resentful and floundering.
“Baby’s Coming: What do you really need?” - one of my favourite postpartum handouts challenges you to think beyond sleepers and diapers to the things that will really make a difference during those early weeks at home. While I’m not suggesting you ignore stocking up on diapers, I do encourage you to ALSO focus on the following postpartum considerations.
Make a Plan.
-
Sleep.
Yes baby needs sleep, but just as importantly, so do you and your partner. Make a plan for not only where baby will sleep (in their own room, in your room, in their own sleep space, cosleeping), but also how you will ensure that your sleep needs are met. This may look like sharing nighttime parenting duties, prioritizing naps during the day, or bringing someone in from outside to enable you both to sleep. I know, I know. It’s so annoying to hear someone say “sleep when the baby sleeps” but it’s such a persistent phrase for a reason. In those early weeks, sleep trumps all. Offload any other responsibilities that you can in order to get enough sleep so you can roll with the other punches. And I promise - it’s a lot easier to have this conversation pre-baby than when you’re both already exhausted and a little emotionally fragile. One option? Have one parent get an ‘early bedtime’ and the other get a ‘sleepin’, offering both of you an extended stretch without having to wake for babe.
-
Food.
Even if you’re not breastfeeding, your body still needs nutritional support to recover postpartum and thrive in early postpartum. While the increase in delivery apps sure makes this easier, best case scenario also provides you with easy access to healthy basics and easy grab options. Brainstorm together what meals and snacks you may want postpartum and how you will make that happen. I’m a huge fan of feeding the freezer - choose a few days throughout pregnancy to make staples and fill your freezer - muffins, protein bites, and cookies go great alongside lasagnas, prepped taco meat, chili, soups and egg bites. This is also a great task to hand off to family members who want to help but aren’t quite sure how. I would personally prioritize options that are easy to eat (one hand grab for the win!) or would be appetizing at multiple times of day. Another option is to source out meal delivery options that you can start postpartum.
-
Household Help.
This portion will look different depending on your own needs. Take a look at the things you do on a regular basis, and plan out for those things that may be more difficult with a babe in arms. Do you have a pet that will need snuggles or walks? A litter box or yard the needs to be pooper scooped? Do you have a plan for getting our your garbage bins or picking up groceries. While you’re not incapable of doing these things during most postpartums, it can take a huge load off just to have one less thing to worry about. Other often forgotten tasks that friends or family members may be able to help with - laundry, entertainment or transportation for other children, or even just rides for yourself to and from appointments or shopping. Simple tasks like picking up groceries feel a lot less daunting when you’ve got another set of hands along.
Support and Resources.
The absolutely worst time to try to research something? When you’re already in the thick of it and feeling like you’re drowning. Do yourself a favour and create a resources list ahead of time that you can refer back to if you’re feeling overwhelmed or in need of support. Here’s a few ideas to start you out.
Postpartum Doula.
A postpartum doula provides in home support during the early days and weeks to ensure you feel nurtured. She will help take care of not just baby, but you, assisting with infant care, emotional support, breastfeeding, meal and snack preparation, light baby related cleaning and more. These are just a few of my favourites.
Parent and Baby Groups.
Sometimes all you need is to get out of the house and be around other people who understand what you’re going through. In the early days and weeks this will be more for you, but as they get older, interaction with others is super important for baby’s development as well - and you get to fill your social cup at the same time.
Therapy.
No matter how well you prepare, and how fantastic your personal support circle is, sometimes it needs to be a bit bigger. There is only strength in reaching out for additional support if you think you could use a hand.
I want to include here the New Mom Checklist for Maternal Mental Health Help. While written and designed to be completed and given to a provider or support person, this can be a great tool to also assess how you’re feeling and which symptoms may suggest that it’s time to reach out for additional help. Always remember that your partner, your doula, and your primary care provider (OB or Midwife) are always here to talk through what’s going on if you’re feeling unsure.

Now that you’ve had a chance to start thinking about planning for postpartum, I wanted to suggest heading over to Dr Kristen’s website to grab her Postpartum Planning workbook. It is an incredible collection of things to consider, presented in a way that makes you feel empowered, not overwhelmed. Work your way through her suggestions, and reach out if you had any questions, or needed more resources.
All About Baby
No matter how long you’ve waited for this moment, it can be overwhelming once baby is actually here. Read on for a quick intro into life with a newborn.
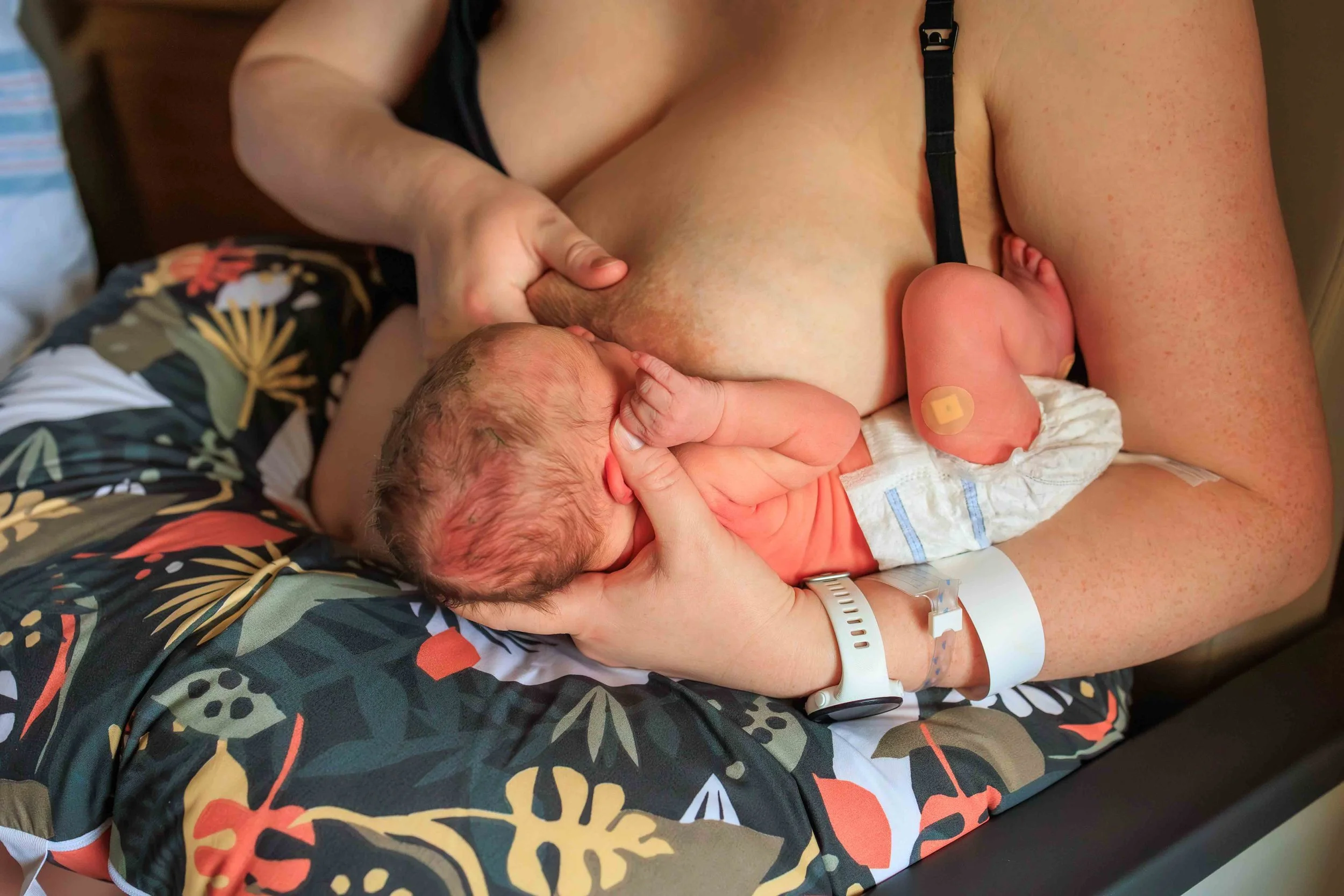
I’m going to post a fantastic video below, but first I want to highlight something that they mention in the video — The first few weeks - survival mode is key. This is not the time to get caught up in all the “shoulds” and outside noise. You want to work on feeling more confident about your chosen feeding method, keeping baby and yourself healthy, and getting as much sleep as you can. The rest of it will fall into place later on. In the video below they do also talk about waking baby to feed - do so to ensure they’re getting enough to eat, but don’t worry about convincing baby into a schedule at this point.
If baby wants to be in your arms and you’re feeling good with it - go with it. You will not spoil or ruin your baby. They are going through huge changes in these early days and will likely be a lot calmer if they are close to you or their other parent, and even better if they are skin to skin. It’s cliche, but soak up these moments, they go by too quickly.
Ready for more? I’m adding an assortment of Newborn Care videos below. Take a peek through as you’ve got time!
Wondering how to care for that umbilical cord?
Infant Sleep
Everyone loves to talk about how your baby is sleeping. It’s an easy topic that seems pretty benign and so it comes up with almost everyone you meet. The problem is that to new parents, it often doesn’t feel benign. It can feel judgmental, and often it just highlights how little sleep you’re actually getting.
I joke that my first baby HATED sleep. And I could live in bed under the covers, so this presented a problem. I spent a large portion of her first year feeling like a zombie, but I also wasn’t comfortable with formal sleep training, so we just kind of trucked along with nothing really working. In hindsight, I wish I’d been more willing to work productively earlier on her sleep. We both would have been a lot happier!
Unfortunately I didn’t have a good handle on what were reasonable expectations during those early weeks and months, and didn’t realize that there were so many more sleep methods out there that didn’t mean just crying it out. It is possible to set a good sleep foundation and build positive habits while still sticking with your parenting ideals. If only I’d known!
So what IS reasonable in those early weeks postpartum? Let’s take a look at normal newborn sleep habits.


There are two parts of newborn sleep that I find helpful to look at. The first will be total hours of sleep. Newborns sleep a lot. But each of them will have a slightly different breakdown for what this looks like for them. If baby is getting approximately these amounts though, that’s a good sign. The second part of sleep is baby’s wake windows. This refers to how long is generally reasonable for baby to be awake before they really should be heading back to dreamland. Too late and you’ve got a cranky, overtired baby on your hands. Too early and there’s not enough sleep pressure built up and baby isn’t sure why you’re crashing their party.
From 0-3 months: your newborn should spend approximated 14 - 18 hours per ‘day’ sleeping. This includes both daytime naps and nighttime sleep. This means they will be awake for only 6-10 hours a day including the times they are feeding and may seem drowsy. At this age baby will likely sleep for stretches of 2-3 hours. In the first six weeks, baby’s wake window is around 45 - 60 minutes. Just enough time to coo at them for a few minutes, change their diaper, feed them and get them back ready for sleep. As they get older this window will increase to 60 - 75 minutes.
Once they get to 3-5 months overall sleep hours will drop to 12 - 15 hours of sleep per 24 hour period. By this point you will most likely notice more of this sleep happens at nighttime, with more defined naptimes during the day. Ensure that they are still hitting those minimum numbers though, regardless of when it happens. By around three months they may be able to happily stay awake for up to 90 minutes before you need to be getting them back to sleep.
What if you’re trying everything but not hitting those recommendations above? I want to share a couple resources that helped me once I finally decided something needed to change. First up, Elizabeth Pantley is the author of the “No Cry Sleep Solution” which was a huge blessing to me when my own babies were little. Not because it provided magical sleep changes, but because it reframed my own expectations and allowed me to consider what should be changed, and what I needed to adapt to for a bit. I was able to make small gentle changes in the right direction. She’s written a mini guide to newborn sleep, linked below.
In my own sleep journey, we never enlisted the help of a sleep consultant, but in hindsight I often wish I had. The truth is that I was never 100% sure I trusted the idea of it, no matter how exhausted I got. So as a doula, I’ve always been hesitant to recommend sleep coaches… until I met Shanel. While I want to be upfront that I’ve never used Shanel’s services, I have followed her on social media for many years now, and I’m continually reassured by the methods she uses, the science behind her decisions, and the way she continually reminds parents that they are in the driver’s seat deciding their comfort level with different tools and methods. She’s the sleep coach I wish I’d known about when I was on the sleep strugglebus with my first baby. So I’m sharing her here with you! If you scroll down her main page you can find a fantastic freebie guide on Five Steps for Early Sleep Success.
I want to reiterate though what Pantley and Shanel and many other sleep experts state — If you are comfortable with your baby’s sleep, and they seem comfortable with it - it’s not a problem. It’s only a problem if it’s a problem for YOU. Like many other ‘bad habits’ (breastfeeding to sleep, holding for naps, picking them up when they cry), only you get to decide if it’s a problem for your family. If it’s not - you don’t need to fix a problem you don’t have.
Co-Sleeping, Room-Sharing and More
I want to start this section with some definitions, so we know what we’re actually talking about. “Cosleeping” is often used to mean sharing a bed with the infant, but actually refers to sharing a sleep space. This does not necessarily mean in the same bed!
Room Sharing is where the infant and parent have their own sleep surfaces, but sleep in the same room. This practice has been shown to have significant protective factors against SIDS and is recommended by all major health organizations for the first six months. Having baby close by can be good for calming your nerves, and is helpful at night when you’ve got frequent feeds as well. It’s a lot easier to only have to walk across the room, than to work your way down the hall to a different bedroom.
Bed or surface sharing is a separate topic, and is a harder one. Research supports room sharing, but does show that bed-sharing is associated with an increased risk of SIDS. There are a lot of factors to this (many of them preventable), so if you are planning to (or think it may happen anyways) bed share, ensure you’re taking a look at the protective choices you can make.
I always said I would never cosleep. It made me too nervous, I wanted my space, and I worried that I’d sleep too heavily. Then I actually had my first baby, and multiple times found myself falling asleep while nursing her in a wooden glider, waking up with a start being completely unaware how long I’d been sleeping. My intent hadn’t been to “surface-share” - but I did, in a highly unsafe situation. We knew a change needed to happen, and so we turned our attention to how to co-sleep the safest way so that I could reduce the risks.
Bottom line - Research shows that the safest sleep is room sharing, on separate surfaces with baby being placed on their back. For some families, this isn’t what works for them, so make the right decision for yourself knowing what the research says and navigating the risks for your own peace of mind. There are several situations mentioned below that are express contraindications to bedsharing - please take note of these, and also the other protective choices you can make if you end up bedsharing.
By the time my second babe was on the way, I knew I needed to set myself up better for sleep needs postpartum. I anticipated having to wake a lot, and needed to ensure that I could safely meet both mine and baby’s needs at night.
For this newborn period, we decided to side-car a crib. It’s exactly what it sounds like, and was the perfect solution for us with both of our boys. This allowed us to room share, while still having our own surfaces. While baby could make their way over to ‘my’ bed once they were mobile, we were able to safely protect the gaps etc same as in a crib, to ensure that they were safe. If you choose to side-car, make sure that the crib is firmly attached to your bed, that there are no gaps between the mattresses (we raised up the crib mattress below before baby got here), and ensure that your blankets and sheets aren’t travelling into baby’s space.

Child Car Seat Safety
Aside from the Breast vs Formula decisions, few things bring up as much anxiety and feelings of judgement as carseats. Which is a shame because in the end, we all just want to keep our babies safe. When we know more, we can confidently do that, as well as confidently respond to any questions we may receive.
One thing I want to tackle right off the bat is that carseat minimums, are just that — not the best case recommendation, but the minimum legal guidelines. In many cases, these leave off far from what the safest option is. I believe our babies deserve better than our minimums (after all, you worked hard to get them here!). First we’re going to look at what the carseat options are.
There are four stages of carseats you will encounter.
-
Rear facing is the safest way to transport your baby, and is recommended until two years of age or until they have maxed out the limits of their seat. Remaining rear facing protects their head, neck and back during accidents since their spines are still developing. In fact some studies go so far as to suggest rearfacing reduces the risk of death or serious injury by up to 92%. Rear facing seats may either be Bucket style (they click into a base, and can be carried inside), or Convertible where they stay in the vehicle and can eventually be changed to forward facing. Minimums state babies must be 22lbs to ‘graduate’, but best case scenario, baby will remain rear facing for two to four years.
-
Forward facing is exactly as it sounds like - a seat designed to face the front of the vehicle. Remember that due to their still developing neck and spine, and heavy head, infants are always safer rear facing if you can keep them that way but may be legally moved forward facing once they are 22lbs. Check your individual carseat, as some also have age (12 months usually) and height minimum requirements. Toddlers should be kept in this harnessed forward facing carseat until they reach the maxmimums of the seat (they can outgrow by either height or weight, check your manual), but legally can move to a booster seat at 40lbs. The majority of forward facing seats on the market today allow for harnessed use until 65lbs. Most kiddos would do best to remain harnessed forward facing until they are between 5-7 years of age, depending on not just size, but also maturity. A harness keeps them in the seat where they are supposed to be, whereas a booster relies on perfect compliance for safety. I don’t know about you, but I didn’t want to put that on my five year old!
-
A booster seat should be used after your child has outgrown their forward facing carseat. Minimum legal requirements are that the child is 4 years old, weighs at least 40lbs and is 40” tall. A booster serves to raise up the child so that the seatbelt falls at the right points on their body, but has no other protective factors - it should only be used when the child is able to ride responsibly and still 100% of the time. If your child is still wiggly, or too short for the belt to sit properly even with the booster, then they should remain in a harnessed seat. Keeping your child in that harnessed seat until 5-7 ensures that when they transition to the booster, they can sit properly all the time, keeping them safe. A booster should be used until the child can “Five step”, regardless of age.
-
There’s a huge rush to ‘graduate’ to each next stage of carseat, and especially so when they’re finally done with them. Unfortunately, many parents move their child up way before they are ready, which puts your precious cargo at risk. Manitoba law states children must remain in boosters until they are at least 4’9, nine years old or 80lbs. In addition to this, look at the Five Step reource in the previous heading. In order to be safest in the vehicle, your child should check of all of these steps reliably before moving to just the seatbelt.
Manitoba Public Insurance has a helpful page here that goes into more details about each of the carseats, and provides tips for installation and usage as well.
Safe In the Seat was one of my favourite resources when my kiddos were little, and she’s still killing it with up to date carseat safety information.
This group is also a fantastic resource for specific questions.
But my baby is too big for rear-facing — their feet touch the back!
This is just one common misconception with car seat safety. Many parents switch their babies from rear to forward facing not because they don’t care, but because they believe turning them is the only option. Let’s look at some of those misconceptions, presented by Car Seats for the Littles.
Infant Feeding
Most parents plan to breastfeed their baby. That doesn’t mean that ALL parents will, or that the process will go as planned. I am a huge supporter of breastfeeding and breastfed all three of my own babies, but let me also tell you WHOLEHEARTEDLY that while breastfeeding may be the best biological option for your baby, that does not mean it is always the best choice for each family. And in the end - the choice needs to be right for your family, not anyone elses. There are a myriad of reasons that a family may choose either not to initiate breastfeeding, to switch to formula and/or bottles after starting breastfeeding, or to choose a combination of the two. If you choose to share those reasons with me, I am honoured. Regardless, I will support your feeding decisions as being the best for your family - because you said so.
With that out of the way, let’s look first at some infant feeding information that is going to be applicable no matter what method of feeding you are choosing.
Signs that baby is getting enough milk
The best practice for most newborn feeding is to feed on demand, which means paying attentions to babe’s hunger cues. Watch your baby, not the clock or the amount in the bottle, and pay attention to their cues. Early hunger cues may be turning their head from side to side, sticking their tongue out, puckering their lips, and sticking fists in their mouths. Crying tends to be a later sign of hunger, and if left that long, it may be harder to get baby calm enough to feed properly. In the early weeks if you can, it is best to limit pacifiers as these may lead to baby not feeding as often. Don’t worry if you can’t (I couldn’t), but make sure that you’re paying extra close mind to the other signs below.
Diaper Counts
In the first week you can typically expect baby to have the same number of wet/dirty diapers as the day they are on. Day 1 you should expect to see at least one wet and one poopy diaper. The poop will be black and sticky meconium (I highly recommend some vaseline on their bottom so it’s easier to get off). Day 2 will see at least two pees and two poops, which will start to turn more dark green. By Day 3 baby should have at least three pees and three poops, the the poop will transition more away from meconium, becoming a more brown/green or even yellowish colour. This pattern continues until approximately day 6 when you will notice the diapers level off. From this point, we should expect to see approximately six or more wet diapers, and around three of them should have some level of poop (note that these do not need to be huge poops to be considered, newborns are very efficient!). If you are breastfeeding, the poop after the first week will often be a light yellow, mustard like consistency, may change with what you eat, and may contain little curds or seed looking bits. If you are formula feeding it will tend to be more consistent, and typically thicker or pastier. Many blogs and well meaning friends and relatives will tell you that it’s normal for breastfed babies to go a few days in between pooping, but recent research suggests this isn’t necessarily ‘normal’ so keep an eye on baby’s temperment and other behaviors and bring it up with your lactation consultant or nutritionist if you have any concerns.
Weight Gain
Alongside those diaper counts above, monitoring weight gain is going to give you your most accurate confirmation that baby is getting enough milk. To start with though, I want you to keep in mind that their birth weight may be overinflated depending on if and how much IV fluids you received during labour. It is normal for newborns to lose approximately 5-7% of their birth weight in the first few days after birth. After this, they should start to gain again, and most babies are expected to be at their birth weight by approximately two weeks old. If your baby loses more than 8% of their birth weight, your midwife or pediatrician will likely recommend watching closely, and if they creep closer to 10%, supplementation will almost certainly be recommended. This can be additional breastmilk or formula, and could take many forms, so make sure to ask questions if you’re not comfortable with the initial suggestions.
After Feed Behavior
While the above two measures should be given more weight, also be sure to keep an eye on how baby seems after and in between feeds. While growth spurts are very very normal, generally speaking baby should seem content and calm at the end of a feed. Their hands will often loosen and open, and they may get drowsy. In between feeds they should seem reasonably calm and able to be settled. If you notice that baby seems just as fussy after a feed as before, or if they’re wanting to feed again very soon after what seemed like a good feed, make sure you’re keeping an eye on their diapers and weight gain. Otherwise, remind yourself that a content baby is usually a well fed one.
Bottle Feeding
As mentioned, most babies should be fed ‘on demand’, which means paying attention to their cues and offering milk accordingly. With formula or bottle fed infants, this tends to settle in around every 2-3 hours, stretching to 3-4 once they’re older and their stomachs have grown.
Newborns may take 1.5-3oz per feeding, but remember to watch your baby, not the measurement. If they’re still seeming dissatisfied, offer more milk. If they lose interest, it’s ok to stop, providing their weight gain has been ok. In the same vein, if baby seems hungry before the 2-3 hour mark, listen to them! As always, if your pediatrician has suggested a different feeding schedule, follow that.


Paced Bottle Feeding
First of all, there is no one best bottle. Let’s get that out of the way before we begin. While there are stronger recommendations for breastfed infants, with the intention to decrease the chance of latch confusion, every baby is going to have a preference for a different bottle. For this reason, I recommend even if you plan to bottle feed, purchase only a few of your preferred bottle type to start - if babe likes it, fantastic, you can grab more. If not, you haven’t spent a years car payments on bottles that will never be used again.
So now that you’ve got a great bottle… how to bottle feed? If you’re like me, you grew up watching babies fed in the crook of a parent’s arm, bottle tilted to the sky, keep going until it’s empty. Seems easy enough, right? While it can be, and some babies do great with this method still, the current recommendation is usually for paced bottle feeding. This allows baby control over milk flow, allowing them to choose how much and how fast they drink, decreasing choking, gas and overfeeding.
For paced bottle feeding you will hold baby semi-upright or sidelying, and position the bottle straight so that the nipple has milk but is not overflowing. Remember to still take breaks to burp and allow babe to decide if they are still hungry.
While we’re discussing best practices for bottle feeding, I want to share this clip as well. Many people think of ‘good latch’ as being only something to worry about when you’re feeding at the breast, but it’s important for bottle fed babies too. Ensuring that baby is getting a good deep latch means less gas, better milk transfer, and less chance of a tuckered out baby before they’ve finished their feed.
Breastfeeding

Breastfeeding is one of those things that people often feel like should just ‘come naturally’, so they don’t prepare prenatally, and then feel badly when they struggle postpartum. Two things can be true. Breastfeeding is ‘natural’ — AND it can also be HARD!
Familiarizing yourself with breastfeeding basics ahead of time can make the transition at birth a lot easier. Thankfully, Lynette at Untied Latch has offered her Expecting To Breastfeed course complimentary for all Winnipeg Birth doula clients.
Click through the link above to enroll.
Click on “Did you receive a coupon of promo code?”
Type in your promo code: JENINE23
Congratulations, you have your course! Reach out if you have any questions, and come back here when you’re ready to continue on.
Lynette has done such a fantastic deep dive into all things breastfeeding that I don’t want to overwhelm you with a whole bunch more details. If you managed to make it all the way through Expecting to Breastfeed though, you should consider yourself well prepared and know that we will tackle any other issues as they come up. A overpreparer like me? Don’t worry, I’ll provide you with a few handouts for additional reading IF you feel called to.
Needing some additional help? Reach out to one of the resources below

